Hyperparathyroid UK
Action4Change
It's NOT All About the Calcium Levels...
Established 02.09.2014
Hyper
Para
thyroid
UK
Action 4
Change

The Truth about PHPT
Benefits of Surgery
-
Significantly improved Quality Of Life
-
Improved bone density/reversed bone loss
-
Reduced/ceased risk of kidney stones.
-
Reduced risks of cardiovascular disease & premature death...
Case stories of people getting their lives back; why we do what we do.
-
Scroll down to read how surgery improves lives, restoring quality of life.
-
Connect with us on Facebook, X @SpSallie, or via our Contact Us page
Jessie Hood
I am writing this four days post op - a successful parathyroidectomy to remove one adenoma, performed by the marvellous Mr Tarek Abdel-Aziz at the Cleveland Clinic in London, and I feel amazing - brighter, clearer and lighter in every way. A totally different person. My head and vision are both miraculously clear. I’m no longer flooded with feelings of anxiety and dread, instantly on waking, I feel calm. The feeling of carrying around a heavy rock inside has melted away, I feel present again rather than detached, as if I’d been living a muffled life behind a smeary pane of glass, and now someone has suddenly unwrapped me and given the glass a good clean! Instead of feeling constantly flat and mentally weary at the prospect of life, I am now remembering what it feels like to look forward to things! Although I am still needing to rest from the op, I no longer have the fatigue, which was reminiscent of very late pregnancy, or the persistent low-level nausea and feeling off colour. Bone twinges have completely stopped, and brain zaps are much reduced Nowhere could I find any mention of these electric shock sensations in the head manifesting as a result of hyperparathyroidism; a common side effect of withdrawal from certain types of anti-depressants, they can arise from the disruption of neurotransmitter levels in the brain during medication withdrawal, but given that hypercalcemia can also apparently affect neurotransmitter release, I am convinced it was responsible for causing these too, along with my other symptoms.
Having read many of the case studies on this website, I know that I have been beyond incredibly fortunate, as from the point of getting a blood test which showed high PTH, to having my operation, was only two months to the day. I am so glad I found the website as it educated me enormously on what needed to happen, and would certainly have given me the confidence to push for the right tests and seek second opinions if I had needed to. Even though I wasn’t in the awful situation of waiting months or even years to get treatment once I had a probable diagnosis, even a week living with symptomatic hyperparathyroidism could seem endless. I had many low moments where the stories of successful surgeries and the encouragement and shared knowledge of fellow sufferers was a lifeline to feel I wasn’t alone or going mad, and that there was something worth hanging on for.
I first felt something definitely wasn’t right at the beginning of this year. I was feeling very low and emotionally flat, unable to feel enthusiasm for anything, and experiencing sporadic episodes of panic, and feeling overwhelmed. There was a permanent low-level knot of anxiety/stress that I had almost normalised, which made me short tempered and occasionally weepy. I had increasing brain fog and the sensation of not feeling as if I was fully present. Getting around the supermarket (and having to repeatedly re-check a shopping list of 5 items) felt like a major and exhausting ordeal. I was unable to find the right words when speaking, and would use the wrong words without realising. I was noticing feelings of weakness, shakiness and breathlessness which didn’t make sense as I was fit and a regular exerciser with a good diet, non-smoker etc. I wondered if a historic episode of depression was returning, though I couldn’t work out why, and due to my age (48), put it down to being peri-menopausal. I resolved to start HRT but wondered if I was deficient in something or anaemic. When I read back the list of symptoms, there were more; such as headaches, palpitations, occasional shooting pains in my legs, it was abundantly clear I was unwell, but as it all came on as a slow creep, rather than overnight, it was difficult to see the picture clearly.
I had a work medical in mid-March and asked them specifically to test my vitamin and iron levels. Everything came back fine - apart from vitamin D which was very low at 26 (51-125). I booked an appointment with my GP in April who listened to my self-diagnosis of peri-menopause woes and prescribed HRT. I asked if she might give me prescription level vitamin D, based on my test result, and she said she couldn’t prescribe anything on the basis of a blood test that hadn’t been done by the NHS, so would instead re-order full bloods and take it from there. I am SO glad she insisted on this!!
The bloods came back and the GP had ordered a bone profile. Vitamin D was still low at 48 (51-125), but improved after taking an over the counter supplement. Phosphate was at the low end of normal, at 0.82 (0.8-1.5), calcium was raised at 2.73 (2.2-2.6), A note from the lab said I should contact the GP within a month to discuss. Two hours on the internet later, researching high calcium, finding the website, I had once again diagnosed myself (but this time correctly!) with hyperparathyroidism. At the follow up GP appointment I already knew what I should be asking for in terms of blood tests, but was worried I might be fobbed off. In fact the GP was brilliant, and suggested retesting calcium, phosphate and vitamin D (advising me to continue with the over the counter supplement) and also PTH. Those results came back in mid-July and showed calcium 2.75 (2.2-2.6), phosphate 0.78 (0.8-1.5), vitamin D 57 (51-125), and PTH 9.8 (1.6-6.9).
At this point I was very lucky to have the option of going privately via health insurance, and got a referral very quickly to see endocrinologist Dr Andrew Bates in London. I was worried he might suggest a ‘watch and wait’, as I had read that not all endocrinologists are well informed about PHPT, but that was not the case at all. At my appointment he reviewed the NHS blood results, said it was highly likely that I had a problem with one of my parathyroid glands that would require surgery to treat, and then ordered more tests for calcium and PTH, and a urine test to determine the calcium: creatinine excretion ratio. At the same time he booked a 4DCT scan and an ultrasound of my neck. Wow! Two weeks later I was back in his office to learn the results. He was unfazed by the fact that my calcium had dipped just into the normal range at 2.59 (2.2-2.6). Vitamin D was 72 (51-125), PTH was 19.7 (1.6-6.9), and both scans had shown the same thing, a 12 mm right inferior parathyroid adenoma. However, because the calcium: creatinine excretion ratio had been low (0.013), he ordered a re-test to discount Familial Hypocalciuric Hypercalcemia, and also a 24 hour urine collection, along with bloods for calcium (again!) and magnesium. In these final tests calcium was out of range again at 2.65 (2.2-2.6) and magnesium was in range at 0.84 (0.7-1.0). My urinary calcium was high at 11.7 mmol/L (2.5-7.5) over 24 hours, and a higher urine: creatinine excretion ratio this time of 0.025 meant that FHH could be discounted, and he made a surgical referral. I was jubilant!
He referred me to a (by all accounts) excellent and experienced London surgeon, but it turned out they weren’t fully covered by my health insurance. The insurance company was supposed to supply the names of three surgeons they fully covered, but only supplied two, one appeared to be a hernia specialist and the other was someone who didn’t seem to do many parathyroidectomies, which I knew was not ideal. I suddenly found myself feeling panicked with the task of finding a surgeon for myself. Once again the website was an invaluable resource as I was able to find names, and read recommendations, which allowed me to make a choice with confidence. I emailed Tarek Abdel-Aziz’s office, outlining my case, and at their request sent him all my previous test and scan results. I had a consultation with him eight days later, and went armed with the questions I knew I needed to be asking, but he pre-empted all of them, volunteering all the information I had been hoping for.
He explained that the scans gave a clear surgical target, so he would start there, and he would do intraoperative PTH testing. If the level didn’t drop as he would hope to see, he would go on to explore all the other parathyroid glands. Continuous nerve monitoring would be in place during the procedure to minimise the chance of damage to the recurrent laryngeal nerve, and my calcium and PTH levels would be tested again after the operation while I was still in hospital. I found him expert, very professional and enormously reassuring. He was also very patient and kind, which felt really important as, in spite of the massive psychological boost of knowing I was on the way to getting better had given me, due to the brain fog I found it difficult to absorb the details of the consultation, so had to ask him to repeat and clarify things a lot. I hardly dared to ask him when all this might possibly happen. When he said he thought he could fit me in the following week, I nearly fell off my chair! He also helpfully organised for me to have my pre-operative assessment tests done immediately following the consultation, as the surgery date was so close, to save me having to make a separate trip into town on another date before the operation.
The day of the operation passed in a bit of a blur, but I felt in very safe hands, and everything went according to plan. My vocal cords were examined just before I was put to sleep, to assess existing nerve function. Intraoperative PTH dropped from 15.7 to 0.5. Calcium had been 2.8 in the pre-op tests. Three hours after surgery it was 2.68, and twelve hours after it was 2.47 (2.2-2.6) – normal!! By twelve hours, PTH was heading back up towards the normal range, at 1.15 (1.6-6.9). Tarek confirmed he had successfully removed a single adenoma and said, ‘you are now cured’. The magic words!
I had one night in hospital, was back home the next day, and almost from day two. I have felt utterly transformed. I am eating good dietary calcium, taking magnesium supplements and continuing with over the counter vitamin D. I have had no tingles or anything to suggest calcium is too low. My voice is unaffected. I feel well in a way that I had forgotten was possible, and better, in fact, than I can remember feeling long before I actually felt ill, which makes me wonder just how long my PHPT had been rumbling away in the background. I’m due to have a post-op follow up (with bloods to be taken beforehand) in a month, and will be referred for a Dexa scan to see what state my bones have been left in.
If my story can help someone make a choice of which professional to approach, or to keep hanging on in there until they can get their surgery, I would be very happy.
Primary hyperparathyroidism during pregnancy
-
We would like to see calcium routinely tested early in pregnancy. Parathyroid surgery is not considered safe during the second trimester.
-
With over 800, 000 conceptions recorded annually in the UK alone, we understand its not financially feasible to test PTH routinely.
-
Consequences of PHPT in pregnancy are increased risks of miscarriage and stillbirth.
-
Both expectant mums and newborns must be carefully monitored if surgery isn't a viable option.
Harj Chana - A very happy ending after PHPT during pregnancy
I was diagnosed with Primary Hyperparathyroidism in February 2019, at the age of 29, I remember the call from my GP at the time saying my calcium levels were high, I had absolutely no idea what this meant and when asking my GP her response was "numerous things including myeloma" at no point did she mention anything about Hyperparathyroidism, however she did say I would need to be referred to the Endocrinology department at Bedford Hospital.
I was worried after the call with the GP. Luckily, I had private health insurance, therefore I referred myself immediately to an Endocrinologist who confirmed that I very likely had a curable disease known as 'Primary Hyperparathyroidism' which calmed my nerves. He went on to advise that my calcium and parathyroid ranges were always in the upper limit of normal which wasn't normal. At this point, knowing the state I was in he also wrote a letter to my GP to complain of the worry they had caused me and to explain to them that I very likely had primary hyperparathyroidism.
Though my Endocrinologist did mention that pregnancy is best avoided until the disease has been cured, I did end up falling pregnant that following month.
My Endocrinologist said I would need to be closely monitored during my pregnancy. He sent a referral to my maternity department and I was handed over to them to look after me throughout my pregnancy.
At my initial appointment with the obstetrician and Endocrinologist, I remember being the only person in the waiting room. From what I understood back then this was relatively rare at a young age, especially in pregnancy. I asked how often this was seen in pregnancy. Her response was 'this is the second case we have seen in the last 6 years.' My heart dropped. I was so scared that no one would know how to deal with my case or look after me. I asked about the risks of being pregnant with this disease. The response was very distressing;
high calcium during pregnancy can risk the baby to be born with low calcium which can be dangerous
Rickets disease in babies
Risk of miscarriage & still birth
They did however have a plan for me and if my calcium was to go over a certain limit (2.83) during my pregnancy would they then need to intervene and operate. So following on from my initial appointment I was to have bone profile blood tests every other week throughout the rest of my pregnancy to monitor the following:
Kidney function
Calcium levels
Vitamin D levels
My endocrinologist would meet with a team of endocrinologists across the board to discuss my case. I was strongly advised to ensure I was staying VERY hydrated to flush out any excess calcium out of my body. From that point I was drinking nearly 4 litres of water on a daily basis.
I was lucky to keep my calcium levels at no more than 2.7 throughout the start of my pregnancy up until 35 weeks, when my vitamin D levels (which were always low) became worryingly low so they decided to put me on vitamin D tablets, I was hesitant of taking them as vitamin D is reported to increase calcium levels, so I knew that if I took them my calcium levels would shoot up, and as expected that is what happened.
At 36 weeks pregnant I went in for my usual blood tests, The following day I went for my routine appointment with the obstetrician and endocrinologist. They said 'you are not going home. We are keeping you in and you will be induced.' My calcium levels had risen to 2.81, bearing in mind the cut off to operate was 2.83, this could have become very dangerous for my baby.
I was in a very bad way and it took a lot of people to calm me down, I was frightened for my baby. We went home, packed a bag and returned to hospital for a long eleven days stay, which was difficult for me mentally, no one likes the hospital experience. There were not enough beds, so they were unable to induce me until they had room. I was placed on a drip to keep my body hydrated to ensure the calcium was being flushed out of me, though my body did not react well to this drip, there was so much fluid in my body I ballooned out, I couldn't even walk due to the fluid swelling. I was on this drip for six days continuously. I had to plead with them to give me a break and allow the fluid in my body to settle. They were very sympathetic towards me, however I was only allowed thirty mins without the drip. Though they did sympathise, there was not a lot they could do as understandably my baby came first. They also had guidance from senior endocrinologists across the board to ensure I stayed on the drip until my baby was born.
On the sixth day, they woke me up past midnight and said ' Are you ready to meet your baby?' I was wheeled down into the delivery room where I was induced. My baby girl arrived and she was born happy and healthy which I am so thankful for. We ended up staying in hospital for a further five days as the team at Bedford Hospital needed to ensure my little girl's calcium levels were not affected. For the first five days of her life she needed blood tests to monitor her calcium levels and the pediatrics team at Bedford would liaise with the pediatric team at Great Ormond Street hospital to confirm everything was as it should be.
On the fifth day we were discharged and after a long eleven days at hospital I was so grateful to go home and see my precious little dog. We were advised that my little girl would then need to have weekly bloods for the first eight weeks of her life, so we did and luckily she was discharged on the eighth week. I am very thankful to the team at Bedford Hospital. Though my case was rare they did everything they could to look after us.
Following the birth of my baby, I went back into the care of my private endocrinologist and was sent for more bloods. At that point. my calcium and PTH levels both rose to above the normal range, so they were now in the higher outer ranges, which confirmed that there was a parathyroid adenoma there somewhere that needed to be removed. I was sent for the following tests:
Bone Density Scan which showed signs of osteopenia luckily no osteoporosis
24 hour urine
Nuclear medicine scan
Ultrasound of the neck
The Nuclear med scan and U/S of the neck unfortunately did not show any adenoma. My endocrinologist advised i would need to be referred to a specialist in Cambridge who would be able to refer me to a more experienced radiographer to search for the parathyroid adenoma.
I was referred privately to the wonderful Mr. Piyush Jani (ENT / Head & Neck Surgeon), Mr. Jani has looked after me ever since (even for non parathyroid related things). He referred me to his expert radiographer who was able to identify my parathyroid adenoma. I had a CT scan to cross confirm. I was then put down on the list for parathyroid surgery.
16 Dec 2022, my surgery took place at The Spire in Cambridge and was a successful, smooth operation, followed by a quick recovery, minimal scaring; honestly a pleasant experience for an operation. I'm very thankful to Mr. Piyush Jani.
Since my experience, I have learnt a lot about Primary Hyperparathyroidism and goodness me it is more common by far, than we think. So many young women are getting misdiagnosed due to GP's not knowing enough about this. The symptoms of Primary hyperparathyroidism can be so generic that people and healthcare professionals are missing it. My symptoms were only;
-
Occasional bone pain
-
Tiredness (aren't we all!)
-
And a few more symptoms here and there that I really would not put down to anything in particular.
Having primary hyperparathyroidism during my pregnancy could have very easily been avoidable had my GP picked up out of range calcium levels earlier on in the year. The trauma of being pregnant and going through this was difficult.
Its a huge thanks to Sallie and the Hyperparathyroid UK Action4change Facebook group that I didn't feel so alone during this. I URGE anyone that feels slightly off to get your bone profile (Calcium, PTH & Vit D) checked as this is far more common then people think.
I know things could have been a lot worse, but this experience has been tough, yet I've definitely come out the other side. I must say it takes a lot to knock me now.

Louise Bower
5 March 2025 - Until a year ago I'd never even heard of a parathyroid. I found out my PTH was high through a random blood test. After looking into primary hyperparathyroidism, it explained all the awful symptoms I'd been suffering for the past 10 years. The best thing I did was to find this amazing group. Honestly I can't praise it enough. You have all given me the strength to keep fighting for myself. I'm normocalcemic. I found myself back under the GP for a 12 month 'watch and wait' after being referred to the hospital. I decided to go for a private consultation, but unfortunately, as lovely as he was, I didn't find him NCHPTH friendly . There was a post in the group from Sallie about a normocalcemic lady, which I saved on my phone along with a comment from a moderator Lesley. Whenever I thought I was going mad (which was every day) I kept looking at them. They gave me the determination to push on. I took the decision to contact Shad Khan for a third opinion. I had a telephone consultation followed by a face to face appointment the week after. WOW... What an absolutely amazing man, so kind caring and compassionate. I no longer feel that I'm going mad and I'm booked in for surgery on 29th March. I can't thank this group enough, if it wasn't for you all I would never have got to this point.
29 March 2025 10.16 pm - Today I realised I do belong in this group. After being told my 'levels weren't high enough', my symptoms were 'fibromyalgia and there's no cure', and 'if it is normocalcemic PHPT, then it's mild, and 'there wouldn't be a gland big enough to remove', I have spent every day questioning myself, and I mean every day, I have cried today with relief and happiness. My discharge notes state, Diagnosis: Primary Hyperparathyroidism. 1 x 1cm adenoma removed. My PTH dropped from 18 to 8 after it was removed. My calcium had ranged between 2.23 and 2.46 over this past year. It's definitely not all about the levels. This group is absolutely amazing. Without it, I would still be suffering. I can't thank you all enough . A huge thank you to some real life angels... Sallie, Lesley and the super talented SK.

Nicky Roberts
Nicky astonished us in more ways than one. His fitness levels obviously stood him in good stead throughout his diagnosis. Whilst most of us are completely floored by hyperparathyroidism, Nicky continued running, and running...
May 2024 - Nicky shared with us; 'I am a fairly new Primary Hyperparathyroidism-er, having only discovered I have the condition in March, after a couple of years with some of the classic symptoms (bone/muscle pain, regular headaches, memory loss among other things). I was admitted to hospital with a calcium of 3.8. I stayed in for the best part of a week and was readmitted last week with a calcium of 3.64. My current level is 2.9. I'm now on 120 mg of Cinacalcet a day, awaiting my surgery to get rid of the misbehaving PTH gland. However, despite this, three days after leaving hospital I ran from Swansea to London, a distance of about 203 miles over four days to raise funds for a local cancer charity.'
What an incredible achievement, despite very high calcium, and increasingly high doses of cinacalcet, the largest dose we've seen anyone prescribed in over a decade;




1 August 2024 - calcium has reduced from 3.35 (July 16th) to 2.95 (July 30th) after increasing the Cinacalcet dosage from 270 mg to 360 mg and a 1 day stay in hospital on IV and bisphosphonates. Good news, but I'm mindful that I took a similar drop, and then subsequent rise again when I was upgraded to 270 mg. Looking forward to surgery now, but glad to be just under that magic 3.0 level once again!We were concerned about the dosage and relieved when Nicky did so well after surgery. Although we expected a large adenoma, we were very surprised to hear about its weight at his six week post op appointment in October.
'Just came away from my first post surgery appointment. Calcium 2.35 mmol, PTH 4.8. My adenoma weighed 6 grams !!'
01 December 2024 - This Saturday just gone marked 100 days since my parathyroidectomy, so I celebrated with a day off work, a little bit of a lie in and then a 45 km long run. Whilst I was very fit before diagnosis and before surgery, I cannot put into words how much better, and how different I feel now compared to that year or two before surgery. I just felt so terrible, so gradually that I fooled myself into believing it was some kind of 'post 40 slow down' or similar.
I've been back at work for about eleven weeks now, running wise I've covered almost 1000 km since surgery, and I've been lucky enough to spend a weekend in Berlin and a night or two away in the UK. At three months post surgery, I'm probably approaching my next set of blood tests in the coming weeks, when they happen I'll share the results.
The turnaround has been phenomenal. No bone pain anymore, one single headache in the whole three months. I can attribute that to a day where I drank hardly any water and about six coffees!. I've lost weight, in a planned manner, and my short term memory is 100% better than it was last year! Another thanks to all on this group. The group has been the guiding light for me throughout this whole adventure. (Only Nicky would call it an adventure, which makes me smile - SJP).
Whilst my surgeon and endo consultant have been great, they didn't really give me any education on the condition, the treatment or anything. I kind of learnt about everything through this group and what limited stuff there is on YouTube. So going from discovering what the hell PHPT was on the night I was diagnosed with it, to being able to chat about my PTH levels and cinacalcet dosages and whatnot with my surgeon has been completely thanks to this group. My aftercare in terms of what vitamins to take, what to avoid etc. has all come from here and I'm sure has been key to me feeling so great now.
For those in the line for surgery, please have hope. I know I'm a good example and I know that not everyone comes out of surgery singing from the hill tops about how their life has changed beyond all recognition, but I can truthfully say that what I feel now is completely unrecognisable from what I felt like in 2022, 2023 and the first half of 2024. Thanks all.
When I first created this site in 2016, our members were concerned about people over 50 being refused investigations for PHPT and surgery, based on their age. Eight years later, we have a new age related concern, an alarming increase in number of teenagers diagnosed with primary hyperparathyroidism. One new member; a 17 year old female was dismissed from A&E as 'an anxious teenager'. She was experiencing frightening cardiac symptoms. She called 111 who took her seriously. She was found to have elevated PTH and calcium >3.00. She found us thanks to Libby posting on TikTok. The very next day we had another new member aged 18 with a similar story. I anticipate teenage hyperparathyroidism is going to increase. The NHS needs to be aware and become prepared.
Libby describes the impact hyperparathyroidism had on her young life from 13 - 15 years.
The feeling of isolation and loneliness is like no other. Being a teenage girl struggling to fit in, whilst suffering with an unknown draining illness, is truly something no one should ever go through. Hyperparathyroidism is a disease unheard of in society, even though it affects many people, especially 'middle-aged women'. Strangely, the last time I checked, I got this life altering disease in my early teenage life, my prime time, the time when I should have been constantly out, laughing and enjoying my life. Instead, these first few teenage years were taken away, exchanged for a life which consisted of bed rotting. At thirteen years old, I was experiencing aches in my limbs, insane migraines and tiredness, which I assumed was normal, as it was blamed on being a hormone thing since I was going through puberty. However, people my age grew out of these pains, but mine were only just starting...

By the age of 14, it was hard for me to get out of my school chair due to intense aches in my lower back. One doctor appointment later and, 'perhaps it’s a muscle issue?' Many tears later, a second appointment was scheduled and a blood test was arranged… high calcium.
By the age of 15, I could barely attend school. My symptoms progressed. Nausea, brain fog, extreme thirst, and an intense urge to urinate frequently at night, which would steal my sleep from me.
“Libby gets to leave school early, all the time for appointments”
“Libby stop skiving”
“Libby why do you always miss school?”
Scans later, the last day of year 10… finally. The 21st of July 2023 was my neck scan, which confirmed I had a benign tumour on my parathyroid gland. Walking into school for the last day before summer after being told I had a benign tumour snatching my life from me was a very strange feeling but I couldn't possibly miss the teachers tug of war! I finished year 10 with about 60% attendance.
The summer flew by. The majority of it was full of bed rotting again, and watching my parents worry about me, even though they did their best to hide it. A month after my neck scan, I went to Florida for a family holiday. What teenager gets tired after being at a water park for about an hour? What teenager struggles to walk around theme parks? Even though I enjoyed my holiday, hyperparathyroidism once again took away some joy.
The return to school, year 11. More and more blood tests and scans, pretty much a doctor or hospital appointment every single week. The word surgery was finally a topic spoken about for the foreseeable future. After the whole of October off school we got some exciting news that I will get to meet my surgeon in November, Mr Hubbard in London. Surgery would be in the New Year. In December, many GCSE mocks were missed due to painful symptoms. Would I actually be able to sit my GCSEs?
Finally, the day comes. January 14th, the day before surgery, we pack our bags and head into London in preparation for surgery the next day. January 15th 2024, my life changing little nap! Waking up knowing that the little benign tumour won’t hold me back anymore. I can finally be a teenager!
The recovery process for me was quite long. It took about a month or so to adapt to my new life. The answer to the question would I be able to sit my GCSEs or not was still unclear in everybody’s minds due to the unsteadiness of my mental and physical health.
18 GCSE papers later! I actually did manage to sit my GCSEs. Six months after surgery (July 2024), I can notice a significant change in my everyday life. Although I still struggle with headaches, life is a lot better for me without my symptoms. Everybody else notices the change too, even boys in my school who I've hardly spoken to!
“Libby’s had such a glow up!”
My family have their Libby back, who was hidden for a while.



Kerrie, Libby's mum;
I want to raise awareness of how awful this condition has been for my daughter. It is sad to think that there's probably so many teens going through the same thing. I still remember the call we received to tell us Libby had a potential adenoma and hyperparathyroidism. It was so scary. I went into another room to ask if it could be cancerous. Thankfully I was assured it would be very unlikely as the rest of her bloods were OK.
Libby was diagnosed at 15, but had been having symptoms for some time before her diagnosis. Libby was 'lucky' our doctor was fantastic, and knew about primary hyperparathyroidism. We were told it's rare in children, but the correlation between the calcium and parathyroid level was evident of primary hyperparathyroidism. Libby went through numerous blood tests, ultrasounds & finally the nuclear medicine scan before being diagnosed.
Life before her diagnosis was so difficult. Libby had bone pain, she was fatigued, she felt nauseous and was low in mood. Libby's attendance at school was poor, she was withdrawn from her peers, and family life was difficult. Libby would come home from school and just go straight to bed. I thought she was depressed. I thought she might have had over or under active thyroid, as I know one of them can cause depression. Then came the back pain. Libby would repeatedly tell me she thought she needed an x-ray due to the pain. Two locum doctors we saw before our family doctor, requested blood tests as it was unusual to have back pain at her age.
Activities were cut short, holidaying wasn't as enjoyable as it should be. Hyperparathyroidism was relentless! One thing I think should be highlighted from Libby's perspective, is how her social battery was non existent, I remember how exhausted she'd feel. We were often the house the girls would hang out at. Libby would come and tell us she was out of her social battery. It was so awkward, but she couldn't help it. She needed to rest and try to hype herself up to do things. Walking ten minutes from the bus stop after going to town was a no no. Walking twenty minutes to school wasn't possible either. It would tire her out. We thought it might have been behavioural at first, but once we found the group and read other people's experiences, it was evident that it was hyperparathyroidism.
Libby had surgery at the Evelina hospital in January this year. The difference is incredible, we have our daughter back. We really missed her! It was a rough few years before we had a diagnosis. Libby sat her GCSEs in May/June. We honestly didn't know if this would be possible pre surgery. We've just had a week away in Greece, it was so lovely, she's great company and very lively now! We hired push bikes (not our best ideas in those temperatures), but we couldn't even enjoy the theme parks in Florida in September.
Sallie and the Hyperparathyroid UK Facebook group has been an incredible source of support, Sallies books are so informative too.



Alfie's Hyperparathyroid Story.
Since 2021, we have seen increasing numbers of teenagers diagnosed with primary hyperparathyroidism. Genetic causes were ruled out. We followed the cases of two 14 year old boys. We felt very sorry they had found themselves dealing with this disease. They were diagnosed at different times, in different areas. They both had parathyroid adenomas removed, which gave them back quality of life. One parent told us it took two years for her son to get completely back to normal. Another parent Natalie, wanted to share her son's case story in the hope it might help other parents to recognise symptoms in their children.
Natalie: Looking back, my 14 year old son had quite subtle symptoms in the beginning. We think his symptoms started at least two years before his actual diagnosis of PHPT (October 2022).
It all began gradually with lack of energy and motivation, and missing matches for his footy team. If he did make it to training sessions he'd complain of pains for days after, he gradually withdrew from a lot of things actually, both physically and socially. His school attendance became quite patchy, "Mum I'm not faking it" he'd say, "I can't explain it but I just don't feel right or well, please believe me and let me stay off." I did believe him but even I will admit that some days it was hard, as there wasn't actually anything physical to see.
As time went on, everything got worse. The headaches increased, foot and bone pain worsened, and he could only complete short walks. Changes to his gait became apparent, and he was saying he felt nausea a lot of the time too. Because he was a transitional age, most of these vital signs that something was wrong, could very easily have been put down to other things; 'maybe he's a bit anxious', 'he's a pre-teen, it's normal', 'it's probably hormones.'
The GP was on the ball though, and referred us to the hospital. It was at this point we started to jump through hoops (lots of them!), and hospital departments, from orthopaedics to physiotherapy to neurology... sadly.'
"The group kept me grounded when I became too overwhelmed, which enabled me to support Alfie much better, as he was now barely in school or really functioning. It was sad to see my boy this way "
Orthopaedics did a full bone profile (Feb 2022), but failed to recognise his raised calcium of 2.77, so we carried on jumping through hoops which held things up by six months. They discharged Alfie, advising him to continue the physio exercises and that things should resolve! Neurology excluded all neurological causes, but did detect the high calcium, and ordered a PTH test which was also elevated.
Eventually in October 2022, Alfie got the diagnosis of Primary Hyperparathyroidism. You might think things would become easier from here - but no, we still had a full battle on our hands, from tests to scans, to hospitals disagreeing, blood tests going missing, the list is endless really, and it felt like this went on forever.
If it wasn't for this group Hyperparathyroid UK, I honestly don't know where we would be now, as there were days it was all becoming too much.
I was so happy and relieved to be able to write in June 2023, 'Alfie is now six weeks post op. He is cured of this awful condition that sucked the life out of him.
He had an 11 mm adenoma removed, which was hidden tucked behind his gullet. It being removal, and normalisation of his bloods, has already made a huge difference. Alfie's symptoms could have gone amiss for years, and been put down to him being a difficult teenager, lazy, always complaining of something.
My advice to other parents would be, 'If something doesn't seem right with your child or teen, it probably isn't - tap into those subtle changes, listen to them, push and push and push to get the correct diagnosis for them. If your child/teen does get a diagnosis of PHPT then I would advise you to do your research, lean on the wonderful support of Sallie and this group, and finally, don't be defeated.'

I'm sure everyone reading about Alfie, can imagine the smiles, laughter, joy and relief, felt by our members as they saw this lovely update from Natalie, which popped up on our screens four months after Alfie's surgery. It was so lovely to see their smiling faces after many very worrying months.
As many of us have said, it's hard enough to deal with PHPT as an adult, let alone having to endure it as a teenager or to watch your child/teenager go through this. Yet we are seeing more and more teenagers like Alfie diagnosed.
"I've now got my very lovely, much healthier, boy back, and his future is looking bright again!"
Late nights, lots of treats, busy days, bike rides, Copenhagen, Sleepovers, out with friends, walking miles, Joined the gym, lazy days and lie ins, attitude, mischief, and a fair amount of (paid)manual work with Grandad too...
What a summer he's had. Alfie's been making up for any time missed! Four months post op now, and you'd never know he's had surgery or PHPT. No complaints from Alfie
Hyperparathyroidism according to Alfie.
" Whilst I was ill, I didn't really know what was wrong with me. I felt sick, had headaches all the time, and was throwing up every now and again too. It got to the point where I wasn't going to school at all. In fact, I even had an online exclusive learning programme set, so I could learn from home. I soon got used to learning from home and quite liked it.
I then got diagnosed with something I needed surgery for. I went to a hospital in Oxford and the nurses were so nice there, they gave me everything I needed! My surgeon was nice, and he was so caring that I even said to my Mum that I would like to go back there!
He found the fault in my neck which he said was hard to find at first, then he took it to the lab so that they could investigate it. I had quite a bit of pain after my surgery, but I went home the next day and the best part was I was allowed to eat ice cream for a whole week!
After my surgery I soon started to feel a lot better. I don't get nausea or headaches anymore. I am able to do more things, and I go out of the house a lot with my friends now too. I couldn't do this much when I was unwell.
I now have a lot more motivation to do things and I am also back in school."
Alfie age 14
Linda Colvin
I'm almost five weeks post op. My scar is very neat. I had my follow-up today, and was discharged by Mr Moorthy with the plan for GP to monitor bloods annually.
Already my bony aches and pains have gone. My energy levels are up. I’m back to Zumba and aquafit classes. I’m peeing far less, brain fog has lifted, no blurry eyes - and my nails are growing for the first time in years. Result!

To all of you still suffering and waiting for treatment, hang in there. I hope you get surgery soon. To Sallie and the other moderators, thank you so much for all the wonderful advice and support. It really is invaluable and encourages so many of us to persist, ask the right questions, push for treatment.
Sarah Cox
That's me officially signed off as cured!! I could not be happier with my treatment by my GP, endocrinologist and Mr Hilmi, here in Glasgow.
Six weeks post-op, and my calcium has returned to 2.38 (from a peak of 2.94), PTH, vitamin D and magnesium are also all normal!
I just wanted to share my positive experience, and thinking of all of you who are advocating for themselves to be treated, or are awaiting tests, scans, surgery etc.
Thanks to everyone in this group, I have felt so supported through this entire journey.
Wishing you all well .
Carol Hughes
It’s 2 weeks post op. The wonderful Alison Waghorn removed my dressing yesterday drained some fluid buildup and revealed my scar. It’s barely visible!
My bloods are good,and I’m feeling like a new me. I have knocked fifteen minutes of the time it takes to do killer Sudoku's.
I just need to build up my stamina before I return to work teaching. I’m 61. Pre-op I felt like an old lady. I thought I had dementia. I couldn’t add up (not good when you teach maths), every bone in my body ached. I lost my balance and fell over many times. I had heart palpitations, I was exhausted and had no get up ad go.
I cannot thank you all on this this group enough. Without you I would never have been able to, or had the courage, to take control of my treatment.

SW
So today is eleven weeks since I had a parathyroidectomy (lower right) and hemithyroidectomy (left-hand side). This was privately with the wonderful Mr Matthew Ward at Portsmouth. A 4 gland exploration was done as well as intraoperative testing of my levels. I elected to go privately as I have pretty bad osteoporosis and have already had two wedge fractures in my spine as a result. My GP had tried to refer me to Endocrinology, but as my calcium was in the normal range despite high PTH, low phosphate, and elevated ALP, they just advised a re-test in January 2025.
Thanks to all the work by Sallie on this Facebook page and the website, I knew there was such a thing as Normocalcaemic Primary Hyperparathyroidism, so sought advice from Mr Ward who organised further bloods, 24 hour urine, an ultrasound and sestamibi scan. This showed the lower right adenoma and an incidental finding on the left-hand side of my thyroid.
Since the surgery, I have been feeling so much more like myself - brain fog and fatigue are improved, joint pain improving etc etc. I have fibromyalgia and osteoarthritis, so I knew it wouldn’t be an instant fix, and Mr Ward made this clear.
However, I was really struggling prior to surgery and am making slow but steady improvements. So thank you Sallie without your work, I wouldn’t have had the information I needed to pursue a diagnosis and treatment.
Heather Meggison - primary hyperparathyroidism and bone density
Hi all, I have received the results of my repeat Dexa Bone Scan and thought I would let you know the results.
My hyperparathyroid history is that in August 2021, I was admitted to hospital as an emergency with very high blood calcium of 3.45 and parathyroid levels of 44.4, following a routine health check blood test. I was totally unaware I had a problem with my parathyroid glands as my symptoms were very mild, so much so that I put them down to my age as I was 63, and very stressed due a problematic house move. I was in hospital for eight days on a drip to reduce my calcium to a ‘safe’ level. During this time, as my calcium wasn’t reducing, I was given a single dose infusion of Zoledronic acid, which did help to reduce the calcium in my blood. I was also given an ultrasound which appeared to show an adenoma, and told that I would need an urgent operation to remove it although I'd have to go on a waiting list.
I was sent for a sestamibi scan which clearly showed the adenoma and at the same time I was given a Dexa Bone scan. Fortunately, I have private medical care, and I had my operation to remove the adenoma the following month. After surgery, my GP contacted me to tell me the Dexa scan had shown I had osteoporosis with a 24% risk of having a major fracture in the next 10 years. This was a bit of a shock as there is no history of osteoporosis in my family. He prescribed Alendronic Acid (AA) to be taken once a week. Before I could take this medication, I fell and broke my right wrist. Due to the pain medication I was taking for the broken wrist, I decided to wait before taking the AA. At the same time, I had a problem with a back tooth that needed to be extracted, however my normal dentist decided that due to the fact that I'd had a Zoledronic acid infusion, I needed to see a specialist dentist as (rarely) there could have been a problem with my jaw following the extraction due to the bisphosphonate.
Thankfully, during this time, my husband and I did lots of research (Thank you Hyperparathyroid UK Action4Change!) about hyperparathyroidism, and we discovered that osteoporosis caused by hyperparathyroidism may improve once the adenoma has been removed without any medication. I was aware that it may not go back to what it was pre-hyperparathyroidism due to my age, but, having read up about AA and the possible side effects etc, I decided to not take AA.
Fast forward to April this year and I asked my new GP if I could have a repeat Dexa scan. (I have moved house and now live in a different county) which he agreed to. At the scan, the radiographer explained that as my previous results were from a scan at another hospital, my results may be slightly different as the scanners are very sensitive.
I received my scan results today and my fracture score is now 12% and no medical intervention is required! My T score for my hip is -0.4 and for the femoral neck -1.0. ( I can’t find my previous scores, but they were much higher). In 2021 my right wrist was also scanned and that was definitely in the osteoporosis range, however they wouldn’t scan my wrist this time as it has been broken and apparently would have healed stronger anyway.
As it stands, I am very pleased that my scores appear to have improved and that I do not need any further medical intervention, although I do have annual blood tests to check to my calcium and parathyroid levels. Obviously, this is my story and it was my decision not to take AA and I would never advocate that anyone should not take AA. Everyone is different and everyone should discuss their diagnosis with their medical team.
Karen Diamond

Hey everyone. It's been a while since I posted but thought I would do a six month update. Honestly - I can’t tell you what a difference this op has made physically, emotionally and mentally. I have been able to do things I couldn’t have even thought about six months ago.
I’ve been away for a long weekend and I have walked around five miles a day. I have had no aches and pains (except my Achilles- but that’s a different story). The brain fog has subsided, my emotions are more stable and I am sleeping through the night - I feel more like myself than I have in over 4 years!!!
So to all of you starting your recovery or waiting for the op - or even challenging any decision making by doctors - KEEP GOING!! It took me eighteen months to get my GP to take me seriously and I waited a further year for the op. At times I was lower than I’d ever been - but honestly looking back I am so glad I continued to fight the GP who was insistent that it was menopause, because when you know - you know.
Good luck to all you warriors - I am with you xx
Suzie Langdon
I just want to share some brilliant news. I was diagnosed with osteopenia in 2013, and told I wouldn't get surgery until I had osteoporosis. I finally had my operation to remove one parathyroid In 2021. I obviously had osteoporosis by this time! I have just had the results of my latest Dexa scan, and I don't have osteoporosis anymore!
Hang on in there anyone waiting. It can work out better in the end.
Janet Cox
A positive post, four months post op. On Saturday, I baked a lovely chocolate sponge cake. On Sunday, our son came to visit. We don’t see him often as he lives in Hampshire. I cooked lunch, we had some lovely conversation, which for once I could join in and keep up with; no brain fog. Our daughter called in with our nine year old granddaughter. We had a a nice afternoon. My granddaughter asked if I was drunk, because I was laughing a lot!
Yesterday both granddaughters came for tea after school. Today, I dropped a 3 kilo bag of bird seed on the kitchen floor, chuckled to myself as I swept it up. Before my op, I possibly would have left it on the floor to grow. In fact, pre-op, I'd have struggled to do any of these things, including the laughing. If any of you are doubting if surgery is worth it, please believe me, it definitely is!
Suzanne Booker
I just wanted to share this photo with you all, and say a big thank for helping me get to this point. I feel so happy and well and I've got my sparkly eyes back. Yippee! I've had my post op appointment today, sixteen days on from my operation at the Northern General Hospital in Sheffield with Mr Balasubramanian. I had 3 adenomas removed and the thymus too.
I've been so ill for so long (at least 7/8 years). I longed for the day I woke up and felt 'normal'. I can feel the benefits already. It's still really early days, but my vision is seriously much clearer, I can think more clearly. I have more energy now. I'm not constipated anymore, I didn't lose my singing voice, I sleep much better and I have got my sparkly green eyes back. My wound is healing really well too. My levels today are; PTH 23, adjusted calcium 2.10 mmol/L.
I'm being mindful as I have osteopenia. I'm only 49, but I've been advised to take daily calcium tablets and have a high calcium diet, daily Vitamin D, yearly bloods at the doctors, bone density scan in eighteen months time. Alongside all of this I am taking the supplements suggested by this group.

I understand everyone's recovery is different and I'm being mindful to still take it easy and rest up but listen to my body too. Trying to have a little walk every day and get some sunshine on my face too. Thank you all for your support. I have to say on my dark days when the light at the end of the tunnel was dim and gloomy, this support group was my life saver, and I hope my positive story might help someone.

One year update
I’m sat reflecting tonight how one year ago tomorrow I had my four gland exploratory operation.
The photo above was taken sixteen days after my operation. The photo on the left taken a few weeks ago.
I just wanted to show you the difference having the support from Sallie, her admin team, this group, and obviously the operation (albeit much bigger op than had been anticipated as scans only revealed one adenoma and I had three glands plus my thymus removed) has made to me.
So on the eve on my first paraversary, I want to give you all hope. To those waiting for operations, to those not feeling brilliant today, keep smiling and keep fighting, love Suzanne xx
Samantha Blair - At Cat Bells Summit
30 July 2023 - Yesterday, I went on my third hike in a row. I climbed Cat Bells, a fell in the Lake District, Cumbria, with a height of 451 meters. I literally had to scramble up the cliff face! This is me five and a half month post op!!
No more afternoon naps or back spasms. No more Diazepam or Cocodamol. Cholesterol has gone down. No more sore throats or terrible flu like symptoms following exercise. No more Omeprazole which I've needed since my mid 20's (20 years). I realised I've had no acid reflux or waking in the middle of the night choking because of reflux which has gone down my wind pipe! My knees didn't hurt yesterday either. I could go on with all the symptoms. As you're all aware, we get so many...

This is why I was so desperate to get better, so I could make memories like this with my girls. My youngest said to me yesterday, 'We do so much together now Mummy, before, you were always in bed'...
Go get a second opinion. I'm sure I would still be suffering and not cured, had I stayed under the care of my local surgeon. Thank you to this amazing group, and Alison Waghorn at The Royal Liverpool
Christine Tomlinson
To all of you waiting for surgery, this is what I wrote in my diary today. Something I couldn't even think about doing before surgery, due to this horrible condition. I'm now six months post op, and loving life again. Hang in there everyone. There is light at the end of the tunnel. Today I'm grateful to be able to walk 2.5 miles (on my own), along my local canal path in an hour and a quarter.
To enjoy the sunshine and a walk in the rain.
To watch and listen to the birds (Blue Tits) singing and feeding in the trees...
To see two Herons in a field
To watch ducks and boats in the water on the canal
To watch squirrels play
To smile and say say hello to passers by and get the same response back
Simple Pleasures are Life's Treasures
Alan Bristow
Its been 12 months to the day since I had my op at the New Foscote under Shad Khan on 1st April 2022.
I can honestly say its been life changing! I have so much more energy and wellness and in the last 12 months. I've managed to climb Pendle Hill in Lancashire, gone coastal path walking in Wales, and released a new album of my music on line. I cant thank SK and his team enough for giving me my life back and the massive amount of help and support I've had from you all, and the new found friendships for life that have been made.
Pre op my adjusted calcium was 2.8 at its highest, and PTH 8.1. Vitamin D was 53. My adenoma was 22mm. I'm happy for you to use this photo if it helps the cause. It's the very least I can offer in return for all the help and support I've received in recent months. Much appreciated.
A link to Alan's new album: Real Life by SAMCITY - DistroKid

Shad Khan, Consultant Endocrine Surgeon at Oxford University Hospitals, changed the lives of these ladies from November 2020 to January 2021, and many hundreds more since then. The case stories below, with photographs of removed adenomas, some with normocalcemic PHPT are collectively an important lesson showing the unpredictability of Primary Hyperparathyroidism. Predictions of what will be found during surgery based on levels and scans are often incorrect, which can explain the high number of failed ops performed by scan guided surgeons. These cases prove levels do not indicate the severity of symptoms or disease.
Please look at the normocalcemic pre-op levels of the ladies below and share them with anybody who says 'Normocalcemic PHPT is not a thing' or that surgery isn't required. Please get in contact with us if you have NCPHPT and are not being heard. Visit our surgeons page to find other surgeons who recognise that Normocalcemic PHPT patients both need and will benefit from a parathyroidectomy. At the bottom of each page there are links to books published by Sallie Powell including 'A Normal Christmas' which contains many studies dating back from 1969 about normocalcemic primary hyperparathyroidism, which is not a new entity or an entity to be ignored.
Sarah Quinn
Pre op calcium 2.76mmol/L, PTH 10.1
Post op calcium 2.21mmol/L
Sarah joined us in Oct 2020 after being diagnosed with PHPT in September 2020, due to elevated Calcium, PTH, and kidney stones. On 18 November 2020, she wrote; 'Surgery booked 30th November with Mr. Khan. I have never been so relieved, excited, thrilled. Feels like my birthday!'

Sarah told us three days after her surgery, 'Hi everyone. Feeling better every day. The site is quite puffy, sleeping well. My eyesight has definitely improved. no bone pain today! Could be pain killers.. I've got fizzy arms and legs so I'm taking calcium supplements which seems to help.
Dorothy Azebiah
Dorothy had been unwell since 2017. She found our website after a failed sternotomy at St Bart's Hospital, where a lymph gland was removed. Her calcium pre-op was 3.03mmol/L which increased after surgery to 4.00mmol/L. Her two daughters were extremely worried for her.
Dorothy had a re-op with Shad Khan, who located this adenoma embedded within her thyroid. She is now feeling well with her calcium level remaining at 2.31, her thyroid is performing well and her daughters are happy to have their mum back.



Anne Mcdonald
Anne met Shad Khan on 02 November 2020. She wrote; ' I saw Mr. Khan today in Oxford. Five years, five different endocrinologists, five different GPs (in the same surgery), two lots of sestamibi scans and US scans, 2016 & December last year, and for the first time ever, after all of that Mr. Khan has given me confidence that I’m not being fobbed off again and that I matter!!
Anne was offered surgery on 23 January 2021; 'I’m very excited but won’t deny I’m also very scared. especially as Covid is so prevalent in hospitals, and I have CKD'

Anne also has osteoporosis. She felt her marriage breakdown was predominantly due to the symptoms of PHPT which changed her personality and energy levels. She told us; Unfortunately this last year my symptoms have worsened greatly. I feel ill most of the time and have been considering giving up the job I've always loved.
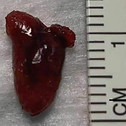
I'm excited when I think about after surgery, and I'm looking forward to feeling like a new woman. Big thanks to Sallie and SK. Without them, I would not be sharing this good news with you tonight.
When I asked her if she wanted to add any feedback about Shad Khan, she replied; 'Oh I’m not great with words Sallie but he has made such a great difference to the lives of so many of us who had given up hope. And even to those who are not able to travel to see him in person, he’s given hope, help, and encouragement at all times of the day and night.
We could go on and on couldn’t we?' Anything I can do to sing his praises I will be more than happy to do. He really is a one-off human being.
UPDATE June 2022: Unfortunately Anne was not cured. Her calcium in may 2021 remained nigh normal, with elevated PTH at 11.6. Her urinary calcium was quite low so she was referred to genetics which ruled out FHH. A repeat pet choline scan in May 2022 however, found Anne had a fifth gland that needed to be removed. She is the fourth member in recent months to be found with a fifth gland, just in Oxford.
Trisha Todd - Pre op Adj calcium 2.9 mmol/L
Trisha had surgery with Shad Khan in November 2020. She messaged us to say she had been told her adenoma was five times bigger than her gland, and shared this photo with us whilst still feeling a bit groggy.
Trisha told me in Feb 2021; 'I'm feeling really well. I've still got Polymyalgia, so a few little aches from that, but I'm sleeping a lot better, and have stopped sleeping during the day. I'm actually doing things again, whereas, before the op, I would just think about them. I can play with my grandchildren again. I'm not running off to the loo every few minutes either. I can follow plots in books and in TV again. I'm back to my usual weight. Quite a lot of improvement for something the Endo initially said could be 'watch and wait'!
This was Trisha, just three days after surgery, looking bruised but very happy and relaxed.


Sue williamson
Pre-op levels June 2020;
Calcium 2.66mmol/L, Adjusted calcium 2.63 PTH 15.9pmol/L (1.60-6.90)
Sue was advised by her endo September 2020,
that as her levels were 'just over', she should avoid dairy foods. After finding our group, she knew this was poor advice. Her subsequent scans were negative.

Shad Khan located all four glands and removed the upper left adenoma 16 mm and upper right adenoma 18 mm. Both lower glands were normal. Her PTH dropped post-op to 1.6pmol/L. Shad Khan told her 'A classic example; Don't rely on the scans!!'
Sue; 'Vindicated and vacated. Very sore throat but the painkillers are working. I'm looking forward to meeting the 'me' that's been missing for the last ten years or more. Mr. Khan... what can I say? Thank you from me and my long-suffering and supportive family who never wavered in trusting me, even when I did.'
Irene Lavin
Pre-op levels: Ca 2.49mmol/L, PTH 7.8pmol/L.
Post-op levels: Ca 2.37, PTH 1.9
Irene joined us in December 2020 and asked 'Is it possible to have all the symptoms of PHPT and a positive scan but with PTH and calcium levels both normal?
Then; 'Having a couple of really bad days. All symptoms getting worse. Then I receive a call from Mr. Khan's team booking me in for my consultation very soon. This wonderful news is the best tonic I could have asked for'

Hi everyone, feeling really good after my op with the amazing Mr Khan! Thanks to you all for all your good wishes and support, it means a lot! I was lucky enough to be in the company of Anne and Claire. It was so comforting to be with them reassuring each other whilst waiting our turn!

Looking forward to being a new woman! Watch this space folks. Forever indebted to Mr. amazing Khan, everyone on here, Sallie JP, and others whose names I can't think of. Still a bit not with it! Love to you all.
Sharon Fairweather-Murray
Sharon had a large adenoma removed by Shad Khan following a failed sternotomy at Addenbrookes Hospital, where a lymph gland was removed in error. Sharon's calcium was 2.68 at its highest. This large adenoma measured 30 mm x 13 mm x 7 mm

Sharon was referred for genetic testing as her mum has also been diagnosed with PHPT. It could be coincidence, and wouldn't be the first time we've seen close relatives diagnosed without a genetic cause.
If you want to share your case story, join our Facebook support group or use our contact page. Positive feedback will help future patients, especially about surgeons who operate on non-classical presentations of PHPT

Anita Kittle - Pre-op calcium: 2.37, PTH 5.9, 9.1, 10. Vitamin D 53
Anita saw her GP in November 2019, suffering from fatigue and headaches, though she'd felt generally unwell for much longer. Within twelve months she had been to A&E several times, had two uroscopies in two months to remove stones from both her kidneys, repeated UTIs, and endured painful stents.

Anita had a previous consultation with another surgeon who felt her levels indicated secondary hyperparathyroidism. Shad Khan offered her surgery because of her symptoms and kidney stones. At a recent catch up with Anita, she told me she has thankfully been stone free for over a year .
Claire Holloway
Pre-op Levels:
March 2020: Adjusted Ca 2.38 mmol/L, Vitamin D 46 nmol/L, PTH 8.1pmol/L, 24hr urine 26.3
June 2020: Adjusted Ca 2.41mmol/L, Vitamin D 56 nmol/L, PTH 10.7pmol/L
November 2020: Adjusted Ca 2.35mmol/L
Vitamin D 59 nmol/L, PTH 8.1pmol/L, 24 hr urine 26.3
Claire had surgery the same day as Anne and Irene. She gave me a running commentary, which was fun. She then went quiet for a couple of hours, before messaging; 'All done, I feel bloody fantastic. A little bit sore but fantastic'. Claire told me, 'Shad Khan and his whole team, including nurses, health care assistants, and anaesthetists are seriously lovely', and said that she had never felt safer.
Claire obviously had NCPHPT, but look at the size of the adenoma removed. Days two and three, she had severe tingles from her mouth to her toes. They eased off after taking Calcichews, drinking milk, and taking magnesium glycinate, which she increased before bed on day three. She had no tingles since keeping up the magnesium and calcium (taken 4 hours apart).
In her own words, 'I always knew something was wrong. I just couldn’t put my finger on it. As the years went on, my brain got foggier, my fatigue grew stronger and the need for a mid-day nap was essential. My anxiety levels were through the roof and panic attacks were a very regular thing. The most recent addition to the symptom list, was heart palpitations, which I had regularly during an anxious episode, but I knew they weren't just down to anxiety when they started to appear on their own.
When I finally got to see an endocrinologist, he noticed my calcium levels had been raised slightly for 18 years. A HUGE thankyou to Mr Shad Khan. The adenoma has now been evicted! If it wasn’t for him I would still be moping around trying to get my doctors to diagnose me with all sorts of diseases. I now feel free. My mind is focused. My bones don’t ache. My emotions are stable. My palpitations disappeared as soon as he evicted the adenoma. I feel marvellous. Now time to go and be 100% me. Nothing to hold me back, no need for excuses, time for me to be me!'


Age should never be a barrier to parathyroid surgery.
Several articles stressing this point can be found throughout our site. Nobody should be denied the chance of a better quality of life because they are over fifty. Or indeed at any age. The reason we mention the age of fifty is that until the NICE guidelines were published in the UK in 2019, leaflets in circulation for over a decade stated only women under fifty would likely benefit from surgery. We still hear it sometimes with the excuse that people under fifty are more likely to have to live with long term damage. Of course many of us women diagnosed over fifty have already lived for decades with undiagnosed primary hyperparathyroidism, misdiagnosed as menopause or fibromyalgia. I would like to introduce you to two octogenarian ladies who were very happy to have their parathyroidectomy.
Jean Lobban.
Meet the lovely Jean Lobban who hates to mention her age but has given us permission to tell you all that she was 86 years young when she had surgery on 17 February 2021 in Oxford. Her surgeon was Shad Khan. Jean was scheduled for a bilateral four gland exploration, although her sestamibi scan, which was done at another hospital suggested a right-sided adenoma, but wasn't very clear. Jean had three enlarged glands removed due to hyperplasia. She was in theatre for thirty-five minutes. Her story and updates were relayed to me by her amazing niece, Maxine Webster.
Maxine told me on 31st Jan; 'My poor aunt has been having a sh1t weekend. She spent 17 hours in bed, She looks likes she could go back now. Tired, in pain, can't concentrate, and gets confused. Made worse she had to get a bit of shopping Friday (I do get worried but she's so independent,) and she came home knackered. Neighbour today knocked on the door at about 2 pm. As I shouted 'we are trying to find her keys', he was waving them at me as she had left them in the door since Friday afternoon, the last time she used them'.

Maxine told us Jean didn't stop talking all the way home after surgery.
Then she stopped off to tell her neighbour all about it for a couple of hours!..
Update 16 days post-op Jean's extreme fatigue and tiredness are gone! Cognitive function has vastly improved. Most of her bad bone pain has also subsided. Her shoulder was so bad she could not even pick up a cup without wincing some days. Both hips hurt her too and they have improved and are not worrying her. She can actually get out of the chair without a real struggle and get up and down the stairs well.
Rosemary Sassoon
February 5th, 2021:
We loved this photograph of Kathy and her mum Rosemary, who was 89 years young in this picture, taken in the car on the way home from the hospital in Perth, Western Australia. Kathy wrote; 'Taking my happy mum, Rosemary, home. She says thanks for all your lovely messages. I’ve read them all to her. Pre-op bloods; Calcium 2.8, PTH 21. Post-op Ca 2.66 PTH 1.3 Happy for now. Two scripts for bloods. One in two weeks and one in four weeks.
She talked nonstop the whole three hour trip home. I’m exhausted and she was still talking as I left her!'

February 22nd, 2021: 'So how is she feeling?
Quite amazed. She had a stroke at 68 and a fall at home four years ago which ended up as a bilateral subdural haematoma, or bleed on her brain. She had an emergency op but the whole thing left her with a leg that wouldn’t respond automatically to the command to lift. She had to think about it first and often dragged it if she was tired.
Immediately post-op the leg was magically lifting by itself and she is now walking further unaided than she has for years. Most of the time she still uses her walker but this is a big difference for her. Her mind has lost its fogginess and she is chatty in the evenings still'.
She Terry
She, had her fourth parathyroidectomy in July 2022. After three previous unsuccessful operations with two other surgeons, She was taken under the wing of Shad Khan in Oxford for her fourth and final op. She had been a chronic kidney stone former, and had given up work seven years ago, unable to concentrate or think clearly enough to drive, and needing pain meds to control stone attacks. She was told she had an ectopic adenoma, but despite countless scans, and venous sampling, no location was determined. She told us she'd pretty much given up hope, and that seeing everyone else get cured was pretty demoralising. Shad Khan was her last hope.
We were all delighted to read her update the day after her surgery. The adenoma was within her thyroid.
Day one Update - 'I was told that post surgery, I would start to feel like the old me again. I worried that after so many years , I didn't know who I used to be, nor if I would even like that new/old me. But I have to say, I love this version of me! I simply cannot fully put into words what today has felt like. It 's been full of smiles, laughter, joy, singing along to the radio, having a little jig in the kitchen, pottering in the garden, and seeing things through new, more appreciative eyes. Yes there have been some low calcium tingles to deal with, but my goodness such a small price to pay.
To everyone who is still striving for surgery, NEVER give up, keep fighting for your cure. And to those who have supported me on this page and who have encouraged me when I lost all hope, look what SK and all of you have done. Thank you from the bottom of my heart. ❤️
Tragically, She was diagnosed with terminal cancer in November 2023. She passed away peacefully on 5th August 2024, surrounded by her loving family.
Emma Glover
'By the time they found my high calcium, I’d just woken up from emergency surgery. I had one kidney failing, three kidney stones, cardiac arrhythmia, osteoporosis, chronic fatigue, and poor memory. I had trouble remembering the simplest things. I couldn’t keep food or water down. I dropped from my normal size 8 to a size 4. I basically spent three months in hospital.'
When calcium levels in your blood reach the high levels mine did, even recalling basic information is impossible. I’d forget a sentence as I was speaking. I couldn’t climb the stairs without sitting down. I was receiving bone cancer treatment to try and repair the damage done to my skeleton, one of the joints in my foot had totally collapsed and has been repaired with screws and a plate. I had so much fluid pushed through me to try and 'water down' my blood, that I swelled up like a balloon, with a 2.5 cm stent inside my bladder and kidney for weeks. Information I was reading online was terrifying. I was scared for myself and also my family. Southend hospital didn’t have a surgeon with the skills to remove the tumour and my levels were rising daily no matter what treatment they tried.

I was told blood calcium of 3.5 can put you into a coma. Mine was 3.33. When I laid down on the trolley on 2nd Jan 2021 my PTH level was 39, at my last check, it was 2.00. So 2020 might not have been the best year, but I’m so grateful for this one thing! If any of these symptoms ring a bell with you ask for a calcium/PTH blood test.'
14 October 2019 - I was rushed into hospital with kidney stones (i have a stent in my left kidney). Doctors ran a routing blood test to check calcium. It was 3.07 mmol/l adjusted. PTH 16.4 pmol/L (1.3-9.3), vitamin D 60 nmol/L. I've been in hospital a week but they've been unable to reduce my levels. Nothing much has been explained and I wondered if anyone could help. Symptoms; fatigue, severe constipation, tinnitus, muscle weakness, loss of appetite, weight loss, depression, fainting, and stones in each kidney. This has been so much to take in this last week I'm so confused.
23 October 2019: I just had my kidney stent removed this morning and The whole thing was covered in calcium deposits. Like white/grey stone residue. The consultant said in all his years of clinical practice he has never seen anyone make calcium as quickly as me. I feel that I’m blessed to have private cover, as that stent had only been in 4 days, and if it was in 6 weeks (NHS wait time) it would of had a huge rock on it, wouldn’t have come out and would have required more surgery.
27 November 2019: Collected the Cinacalcet this morning, the hospital called, my calcium is up to 3.25 mmol/L despite 2 pamidronate infusions, and 3 litres of fluid last Thursday. Anyone feel like they are fighting a losing battle? Pamidronate Infusion no three this week now.
03 January 2020: 'I got my bloods back: Calcium 2.37, PTH 0.6. If I’ve got tingly face, wrists and hands how many Rennies should I take? I ate some cheese but it didn’t do anything. I can’t drink milk. I didn’t see FP today, no medication, no instructions not even a phone number to call for advice. I’ve found some indigestion chews (800 mg calcium carbonate) I’ve taken one but nothing happened as yet, I’m still fizzy.'
Emma wasn't discharged with any calcium supplements and told to take paracetamol if needed. With calcium so high pre-op we had advised her to order supplements just in case, because we see regular occurrences of people post-op, experiencing symptoms of calcium crash which can be quite an alarming experience after surgery.
04 January 2020: After a really bad night, full migraine type pain inside my head & behind my eyes, pins & needles & shakes I was almost ready to go A&E. Amazon arrived with my supplements. Took 3 calcium chews, 2 cocodamol, a migraine patch, and a magnesium salt bath I feel a little better. I emailed FP too, reassurance that the pain I’m in is normal at least. As always, couldn’t of done it without you guys. I wish I could say more than thank you
28 March 2020: Hey guys, just a quick hello and update from me. I’m now twelve weeks post op. I literally feel like a new person. I’ve had an iron transfusion, am now on B12 injections, and my overactive thyroid following surgery has corrected itself. (PTH fell in surgery from 38 to 5). I can now eat without vomiting, I don’t wake up exhausted every day, the kidney pain is gone.
I feel more like myself than I have in the last ten years. I can’t tell you there was one morning where I woke up 'better', it’s more of a gradual feeling. The hospital forgot to test PTH & calcium in my last two blood tests, but I got a calcium result back this week and it’s 2.42 which I think is pretty good!
Margaret Kressinger
Margaret joined us in March 2018. Ultrasound and sestamibi scans in April, were negative. The radiographer suggested if she did have an adenoma it was a small one. Her endocrinologist said surgery would be unlikely with negative scans. In June, she was referred to an ENT surgeon. Her calcium had dropped from 2.8 to 2.73, which her endocrinologist felt was because she'd began taking vitamin D. Her PTH ranged from 16.2 to 17.4 She described painful feet, making her life a misery, feeling drained, with dreadful energy levels, weak legs, dry skin patches, poly urea, trembling hands, sharp stabbing pains, feeling faint, and vision disturbances
In August 2018 she had a contrast CT scan and more bloods. She was offered medication to reduce her calcium. She said she wanted a cure, not a suppressant, and hoped surgery wouldn't be too long after the scan. By November, her calcium was 2.85, PTH 19.1. Her first appointment to see surgeon, Tass Malik, came in March 2019. After her appointment, she wrote 'what a super man, he's put me down for an op. As nothing showed on any of the scans, he's going to do a three hour op and search for them all. I'll have to stay in overnight with a drain. About a 3-4 month wait as he's the only surgeon. Obviously, if he gets an influx of cancer patients they will be his top priority and it will take a bit longer but I'm happy with that. I have put up with so much pain the last couple of years, what's a few months?'
By June, Margaret was experiencing cramp type pains in her hands and feet, and mobility problems with her shoulder. She had a pre-op assessment on 03 July and was given a surgery date for March 2020 by a clerk who told her 'the surgeon deals mostly with cancer patients, (of which she was well aware ) and although she may be in some discomfort at least she didn't have cancer). Her surgery date was cancelled two days before, due to Covid 19. The endocrinologist during a telephone consultation in May, reassured her she hadn't been forgotten. She was offered a new date at short notice due to a cancellation, 25 June.
Margaret gave us regular progress updates. She felt tired the first week and experienced muscle spasms in her neck. She wrote: 'I'm nine days post surgery now and last night was the best night's sleep I've had in years, from 11 pm to 7 am with no waking for the toilet or walking with a bad back. In fact, my body is feeling pretty good! I'm beginning to feel more like me! So good to wake up with no back pain'. Photos below are Margaret at day one and a month after surgery.


'Hello everyone, I've seen Mr Malik. He's very pleased with how the op went, though he said it was a very difficult operation. He removed a parathyroid which was lodged in my thyroid and only took a small piece of thyroid gland away .
My calcium levels the day after surgery were 2.5 originally 2.85 and PTH was 2 originally 29.
My calcium was tested 2 weeks ago and it was 2 .26 .
He wants me to have bloods taken again for calcium and PTH in 8 weeks time . He also wants me to write him a letter telling him all my symptoms before the op and how they are now as he's very interested in the Parathyroid . I think he's an amazing Surgeon/ Consultant, and would fully recommend him. I'm feeling really pleased after suffering for so long.'
James Bates
James suffered chest pain and blackouts. His calcium reached 3.26, yet he still had to wait fifteen months for surgery, after initially being told 6-8 weeks.
Before Saturday 14th July 2018, a day I'll never forget, I was a healthy 19 year old who did a lot of running in my spare time. I ran a 5k Park Run every Saturday morning plus various other races including 10ks and cross-country with my running club. Occasionally I’d complain about my legs hurting (not surprising) or having a headache. Mum would point to the paracetamol. The day started with me feeling great, ready for a competitive Park Run about 15 miles away. When I started running I felt fine and determined to beat my personal best. At roughly 3K in, I felt a pain in the center of my chest. I thought it was my lungs working too hard and decided to slow down which was fine until I sprinted across the finish line. A sharp pain shot through my back, with a headache and light-headedness which took me to the ground. Thanks to my amazing running club friends I had a lot of support and an ambulance was called. Whilst waiting for the ambulance the pain got worse causing me to pass out multiple times. I managed to ask the paramedics to take me to Wexham Park, the closest hospital to home rather than the nearby Royal Berks in Reading.
At A&E, I had another ECG and was seen by a cardiologist. Blood was taken, and I was given painkillers. Having found raised troponin in my blood, I was sent for a CT angiogram. There were no blockages in the blood supply to my heart. The doctors didn’t seem to have a clue what was wrong and admitted me to the GP unit overnight, then moved me to a ward in the morning. More tests followed, which showed corrected calcium 3.01, PTH 17.3 and vitamin D 37.6. I had an echocardiogram, pituitary MRI, got moved to the cardiac ward to await being taken to Royal Brompton for a heart MRI, but the appointment was cancelled. I did two 24 hour urine collections, the label wasn’t filled in correctly on the first one. They found my afternoon cortisol level was undetectable and after a short synathen test which confirmed early cortisol deficiency, likely primary adrenal failure (Addison's), I was prescribed steroids.
An endocrinologist said I had hyperparathyroidism and would need a Sestamibi scan, neck ultrasound, DEXA scan and kidney scan, as outpatient appointments, then surgery. I decided on Charing Cross for surgery. The endo reckoned I could have the operation within 6-8 weeks (ha ha). I was moved to the endocrine ward and there followed days and days of trying to get my calcium level down. I’d be put on a drip, level would come down, off the drip it’d go up again. My 20th birthday was coming up and I wanted to be home by then. I had to rearrange my driving test date. If the calcium went down to 2.6 I could go home. It didn’t go down. I was given a Pamidronate drip and finally the day after my birthday the level dropped, and after 17 very long days I was free to go with a prescription for Cinacalcet twice daily, steroids and thyroxine, to be followed up in the endocrine clinic in 4 weeks. I had more blood tests mid August after which the Cinacalcet was reduced to one a day. Sestamibi showed increased uptake of tracer on the RH side of my neck. In September an ultrasound showed a parathyroid adenoma. An endocrine clinic appointment coincided with my being at college 100 miles away so mum rearranged it. I didn’t actually see the endo again until Feb 2019.
I received an outpatient’s appointment at Charing Cross for 11th December. I was now back to running again but nowhere near as much as before. On 8th December I ran the local 5k Park Run. Afterwards, I went to the clubhouse and was sat chatting to some friends when I blacked out. I was laid on the floor and an ambulance was called, I was taken to Wexham again. Blood tests showed my calcium was 2.98. I spent the next 24 hours on a drip. While in A&E, a endo consultant asked if I had been tested for MEN1. I hadn’t, so he asked another doctor to get the ball rolling on that. I was discharged the following evening and Cinacalcet was increased to twice a day. We went to the appointment at Charing Cross and were seen by one of the endocrine doctors who went through everything and told us the waiting list for the op was about a year but for urgent cases they could do them in 4-5 months! The doctor disappeared for ages and came back in with Mr Palazzo who said I would be put on the list but they needed MEN1 results and the scans to decide what kind of operation they would do.
Jan 2019 I was tested for MEN1, the result was negative. The Short Synacthen Test was repeated. The responses were normal and I could stop taking steroids. They never found any satisfactory explanation for the previous low Cortisol levels. In February I had a heart MRI,which was normal. I was discharged from Cardiology. In March I had shingles. In May I had a kidney scan, no evidence of kidney stones and a DEXA scan confirmed osteopenia.
Mid July I was thoroughly fed up waiting for an op date and asked my GP to refer me to Wexham Park in the hope that would be quicker, but would take whichever hospital came up first. I got an outpatient’s appointment for the middle of September. Out of the blue 3 days later Hammersmith Hospital rang to arrange a pre op on 27th September and op date of 10th October. At the pre op appointment they seemed concerned about my heart, probably because the ECG said ‘fail’ on it and wanted me to go back for an echocardiogram. Mum asked, if the echo dept at Hammersmith would do it that day and they did (yay!). My heart was fine.
10th October came. We got up at 4am and arrived at Hammersmith Hospital about 6am, was admitted at 6.30, saw one of the doctors and was in the hospital gown and compression socks by 7am. I thought I’d have had the op shortly after. How wrong was I, I finally got a bed at 4.30, went down for the op at 5pm and arrived back on the ward just before 8, a single adenoma was removed.
Apparently I ripped the cannula out of my arm when they woke me up, and made quite a mess. Mum and dad went home and I finally got to eat. I was starving!
i was discharged at noon the following day, already feeling better. Calcium was 2.52 and PTH 0.4. At a follow up appointment calcium was 2.38 and PTH 7.

8 weeks post op

1 year post op
I’d describe myself before, during and after PHPT as follows:
Before: I was content, determined to get better at running, enjoyed socialising, positive, wanted to do well and participate.
During: Pain, upset, lost, depressed, lonely, felt like the end, hated myself/everyone/everything,
Waiting: Depression, seriously couldn’t be bothered, basically given up, felt useless, unhappy and had dark thoughts
After: Much happier, determined, sociable, wanting to get on.
Rebecca O'Connell
In August 2019 (aged 38) I started to get unexplained pain in my coccyx. Although I've suffered from lower back pain most of my adult life, this was new and unexplained. I experienced extreme mid-back pain one night, which stopped me from sleeping. The pain slowly migrated to the front. I was also feeling generally unwell, nauseous, and vomiting for no obvious reason. Everything seemed to point to the gallbladder. An ultrasound in October was clear. The pain persisted under my ribs, coincidentally I got a chest infection which the GP concluded was the reason for the pain. January 2020 I saw a different GP. I still had abdominal pain, back pain, and was generally feeling unwell. A full blood panel flagged high calcium. After more blood tests and an ultrasound which showed ‘something’, I was referred to an endocrinologist with a working diagnosis of primary hyperparathyroidism. By this time, I had found Hyperparathyroid UK Action4Change. I knew I needed surgery and that I wanted Mr. Peter Truran at the RVI Newcastle to operate.

My health was deteriorating. I was extremely fatigued, suffering memory problems and brain fog. I wasn't sleeping, and I was in pain. My calcium ranged between 2.55 and 2.73. PTH never reached 10, but they were both inappropriately raised consistently. My vitamin D was very low. My endocrinologist prescribed 1600 IU. He was understanding and referred me to Mr. Truran in March (just before lock down). By this time I was feeling terrible and really struggling with work. My GP gave me a fit note to do half of my hours for four weeks. Subsequently followed by an occupational health appointment who could see the huge impact on my health and well being and that surgery would hopefully be a cure. I was put on reduced hours until surgery.
My symptoms just got worse. I had a headache most of the time, muscle spasms every day and bone pain most days, but even with all of these symptoms, I questioned myself all the time, especially on good days. Was this all in my head? Peter Truran agreed to operate. I wasn't expecting it to be soon due to Covid, but in October I was offered a date for 6th November. I was so excited but also terrified the NHS would stop doing routine surgery again. By mid October I felt so poorly, I could no longer work. I felt like a shell of my former self.

When I came round after surgery and the drugs wore off, I felt instantly more connected with the world.
As I write this I am 7.5 weeks post-op. Today I have been for a run, walked the dog, and been shopping. I’ve watched a film, and at 9 pm I’m sat writing this and still alert. All this would have been impossible for me to imagine just eight weeks ago. I was useless after 8 pm and I certainly wasn’t running.
Hyperparathyroidism stole my life, but surgery has gave it back.
I'm almost symptom-free now. I still get tired, but think that's probably from doing more. I get the occasional headache. I returned to work four weeks after surgery and will be back to full-time hours in January. My family, friends, and even neighbours have seen a notable difference in me since surgery. My energy levels are much higher.
Camilla Oates

I'm now just over 4 weeks post op and feel so much better, I can't actually believe it. No one believed how poorly I was pre-op, and I got tired of trying to justify to people how I felt. No one could really see what was wrong, apart from I was drowning in depression and anxiety so severe I thought I was going to end up dead at one stage as suicidal intentions were so high.
I also had horrendous bone pain, tiredness, bad tinnitus, and was going to the toilet a lot. I went from being super active in the gym, to feeling like I was dying and not being able to move. I got more unwell in the last 3 years. My consultant said I could have had it 10 years. I would sleep for hours and still be tired. Because I had become so inactive I put on a lot of weight.
PHPT had taken over my life. It was picked up by accident in May last year by high blood calcium after I had labyrinthitis. An ultrasound showed I had one adenoma.
Fast forward to April 2018 after surgery, I found out there wasn't just one, two were taken on the left side and my thymus was also taken out. As soon as I woke up, although very groggy I felt like something had been lifted from my body. I felt like the weight I'd been dragging around for years was gone. I felt happy despite just having major surgery, I literally felt amazing. I was sore for a few days after and had a few issues with low calcium but nothing calcium, vitamin D, and magnesium couldn't sort out.
I feel amazing. My anxiety and depression have improved already within 4 weeks. Everyone has said how different I look, my face is less swollen. Writing this has made me cry happy tears because I still can't believe how different I feel or how the parathyroid glands can cause someone so much grief. So if you're waiting for surgery please don't put off having it. I have so much more energy now I'm now back at the gym. That severe brain fog does lift too. I feel like my surgeon has saved my life.
Clare Victoria
August - December 2018
-
So after every blood test since September, having high blood calcium with normal PTH, a referral to Endo at Nottingham NHS treatment centre, where the blood test they did, came back normal, so they sent me away with high dose vitamin D, more high calcium blood tests, and a re-referral to the same Endo, I finally have a diagnosis. Now got appointments for sestamibi scans on 23 Aug and ultrasounds of thyroid and renal tracts on 06 Sep, but follow up appointments not until 26 Oct. I’m lucky that we know I probably haven’t been hypercalcaemic for more than about 3.5 years, so I don’t know how much of my depression and fatigue is related and how much is just life!
-
Today’s brain fog fail: I discovered when I was getting dressed after my shower that I’d only shaved one leg...
-
Today has mostly been sponsored by the letters M for migraine and N for nosebleeds... Think weekends need to be longer to accommodate days like this!
-
Finding it really difficult at the mo dealing with the uncertainty about when this op will happen. I’m usually fine with just waiting but the anxiety’s already got its claws in my brain making me edgy about everything.
-
Over the last week or so my appetite has completely disappeared (I’ve lost 3lb) and my sleep pattern has got really bad, so I either sleep till midday or wake up at normal time but still need a 2hr nap at lunchtime. I don’t know if it’s the phpt, hypothyroidism or depression.
-
Oh wow the heartburn is bad tonight! Nothing is working...
7 April 2019: I Completed Lincoln 10K this morning in 1hr 39min 42secs. Tomorrow will be exactly 11 weeks since my gremlin was evicted. I’ve never even done a 10K before! It is amazing what you can do if you put all that perseverance and stubbornness that you learn along this journey to good use...
John Dennick
August 2017:
Hi all, I'm new to this group I've been reading some of your stories. I had no idea how many people struggled to get a timely diagnosis/treatment. I was diagnosed earlier this year after being hypercalcemic for 14 years! I actually work in the laboratory myself and had to lay the facts out to my GP who has referred me to every Tom dick and Harry under the sun other than the one he should have; (endocrine). My symptoms have worsened steadily over the last 14 years resulting in me being unable to work for the past 3 months. I also have a slipped disc, bilateral sciatica and a dysplastic hip on top of my parathyroid symptoms. Bone pain has become disabling now along with a terrible memory and very poor concentration. I'm a mess basically but am now on the road to getting it sorted hopefully. It's a real comfort to know there are so many other people struggling with this disease and experiencing similar issues. One thing I've learned over the last decade is that this is a relatively poorly understood disease with vastly underestimated effects on patients. I hope you are all well and thanks for letting me join.
Fast forward to 15 December 2017:
So, I'm 4 days post-op. Feeling sore and tired but overall much better than pre-op. I'd say 80% of my bone pain is gone. Headaches, heartburn, sinus pain, stomach pain and bloating have all but disappeared. I've lost almost 6 inches off my waist and I'm eating very well. Mentally I'm a million miles from where I was last week. Still a bit foggy at times but that horrid feeling of feeling bad for no reason is gone. This by far has been the most dramatic change post op. My kids have their dad back, my saint of a woman has her man back and I'm happy actually happy. My fingernails which used to shatter when I clipped them are now as they were when I was a teenager. It's a minor thing but being able to actually see calcium going back to where it should be instead of it leaving and causing problems is very reassuring to me. I've been very lucky to have a positive and immediate response to surgery. Roads for some will be long and complicated but we'll all get there in the end. I hope some of you pre-op/struggling to get treatment/diagnosis will find my case helpful and reassuring. There is hope 😀
Lynsey Ferris January 2017

I'm exactly 4 years post op today so thought I would share my before and now pictures. Within a few months of my op family and friends remarked how I looked brighter and younger.
I think it's important to be realistic about what the outcome of the operation will be for you, it does get better, but it takes time. For me the only symptom that I know resolved with the operaton was polyuria. This meant I could sleep through the night without interruption. That had the knock on effect of better concentration, and more energy. More energy meant I could start to push myself to do more, and as I became more organised my mood improved... Lots of small changes that eventually made a big difference.
I haven't posted since I joined 2 years ago but I try to comment when I feel I can help someone, and I am grateful for all the insight and knowledge I have gained since being here. I also plan to take the letter from the group to my next appointment as I'm sure there are GPs at my practice who will find it beneficial. Thank you all
Elizabeth Mason
Hello everyone! I'm 2 weeks post op and I just wanted to say thanks to everyone for their support over the last 2 years that I waited for this surgery.
When I woke from surgery, I instantly felt like a weight had been lifted from my shoulders. That constant headache was gone, that fuzzy brain feeling was gone and I felt better than I had felt in a long time!

I've only improved every day, yes I have times when I get all tingly and when I feel tired and think is this normal? But I take my calcium and remind myself I'm only 2 weeks post major surgery and my body is taking time to recover!
All blood tests have returned NORMAL! My Endo was so pleased last week when I saw him. My scar is good, almost healed up and I see my surgeon next week hopefully!
To anyone who is waiting, this is nothing short of a nightmare, but keep your head high and your heart strong because when that elusive op date finally comes through your door it will be the beginning of a new life for you.
Zane: "Almost 7 weeks post-op and feeling fantastic. The tingling on my hands and feet have gone, I am sleeping so much better than before. The pain I used to have in my legs has gone. My head feels clearer and able to focus. I had such a heavy fog cloud before; getting up was a chore in itself, making something to eat was effort. I never knew something so small could affect your life in such a huge way. I never thought I would see the day when I would be writing this and saying how amazing life is now. I did a run this morning, a full run around my block and completed it without stopping or feeling out of breath, that was a massive achievement for me as before I couldn't even walk far without feeling pain or my back crumbling with pain."
Catherine Clarke
My daughter found your website which has helped me considerably in finding a reputable & experienced endocrine surgeon. In 2016 a functional practitioner said my calcium levels were raised & a blood test from the GP found elevated parathyroid levels. Three months later an endocrinologist said because I did not have any symptoms, he would ‘play my condition by ear.’ No further appointment was suggested. Three months later my daughter sent me your website - I returned to the GP & said how do I know whether one of the parathyroid glands was cancerous or not? And asked for a neck scan, which showed two nodules, then a further scan was done which did not indicate the nodules were diseased parathyroids. I asked to see the endocrine surgeon & six months later the team decided I had a rare condition that necessitated diuretics and a referral to the ‘bone doctor’. There was no mention of an operation to remove the offending gland.
Meanwhile, I asked the GP for a second opinion at a different Care Trust & saw David Chadwick. A week ago he removed the offending parathyroid gland & also the thyroid nodule. I have more energy, less brain fog, less anxiety & depression & my skin on my hands looks less like fish scales as each day goes by. I have been told it will take three months before my body will get back to normal.
On reflection, I reckon I have had hyperparathyroidism since 2010. I found the following helpful whilst I was waiting for surgery:
-
Drinking copious amounts of fluid daily
-
Increased Vitamin D and Boron when my depression came overbearing
-
Magnesium taurate & Vitamin K2
-
Ensure the endocrine medical secretaries know how to access scan results from a different Care Trust (they have to be applied for)
-
Check to see whether the medical secretary has made a pre-operative assessment if one has not been sent after one month.
-
If surgery has been cancelled by the Care Trust, check with the medical secretary for the next surgery date.
I am so grateful to your website & also to David Chadwick & his team at Nottingham City Hospital.
Susan Rooks
'I'm five months post op and feeling so much better. I'm feeling a massive difference waking up in the morning, and a lot more energised. I still have some tired days - When I had my adenoma removed I had half my thyroid taken as well and it's still taking time to settle down. Still my life is 100% better than what it was before. Keep pushing for that op people! Xxx
Pictures taken August 2016 and March 2017.

29 December 2018:
Hi, I don’t know if this is parathyroid related but I’m three years post-op and have now developed secondary breast cancer and currently under investigation to find the primary source elsewhere in my body. I’m convinced the damage was done during six years of waiting for my parathyroid surgery.
I was getting my life back but then I got triple negative breast cancer in my breast and nodes. Thought at first there wasn’t a treatment option but they turned it around and I had six months of chemo followed by surgery, then 25 sessions of radiotherapy. Responded well and after a year of treatment I’m just starting to feel a bit more energised.
Carie Ridd - Photos before and after surgery and only 12 days apart.
Operation January 14th 2016. Two glands on the right side removed. 'I felt great straight away, and from week to week my energy and concentration levels have increased. I've lost weight due to increased energy levels, and getting out and about more, so that was a bonus. I'm so glad I had surgery. It really did change my life!'


Pia:
The issue of mental health was worst for me. I could not speak in full sentences, could not find words and names, forgot where I had put things, could not find my way in the car. I am sure this is why I lost one job, got another and gave in notice because of feeling unwell. At my first consultation with the endo I asked about this and she said she could not promise progress post op. I cried with frustration.
However, post-op I started a blog to test my abilities and focus. I graduated in Project Management, 2 exams with good results. I started as a freelancing project manager just over 2 years since surgery.
Landess Robertson - Brown Tumours
They are tumours in the bone caused by extreme levels of PTH.
They are extremely rare, some people will have them and never know. They show up in X-rays and bone scans. Large ones can cause weakening of the bone (I've heard of people having broken bones because of them). Normally when your PTH returns to normal levels they will shrivel and disappear on own and no further treatment is required. I had 3 removed that burst through my gum ( how I was diagnosed) but I had a stubborn one deep in my jaw bone that hadn't reduced once my PTH returned to normal. It was weakening my bone and causing pain so my facial surgeon decided to remove it so that the bone can then repair.
Jules had surgery January 2016.
It was her third attempt after two previous dates were cancelled. Her second cancellation left members feeling her raw pain and desolation as she wrote that she was standing outside the hospital in tears.
18 February 2016 - 'Surgery has given me my life back. It's hard to believe how something so small can cause so much disruption to your body and your life. Looking forward to a pain-free happy future.'
Linda Powell - September 2015
It's exactly one week since my surgery. I feel reborn. My bone pain is gone. Stomach pain and constipation disappeared. It's wonderful. I still have a stick to walk with as I have had two spinal surgeries. I have RA. But I have to say that I feel fantastic and haven't felt like this in four years. I'm writing this to reassure people, and say do not to give up hope. When you have this operation, you won't know yourself. Best of luck
The level of calcium does not determine the severity of symptoms...